The most difficult thing about residential care work
Oct 2023
Written by Glenys Bristow
The most difficult aspect of working in residential care is not managing the behavioural challenges of the children and young people, the demanding shifts, or the lack of resources. Rather, it is the surge of feelings that can surface while doing the work. Even calm, caring, and sensitive residential care workers can often be shocked by their own anger and hatred.

A quick desktop literature search reveals a dearth of relevant literature regarding managing feelings of hate and anger towards young people sharing the life-space with residential workers. And yet, anecdotally, we are aware of the many times it occurs. Further anecdotal evidence suggests that workers are too ashamed and fearful to admit to feeling these emotions and seek support.
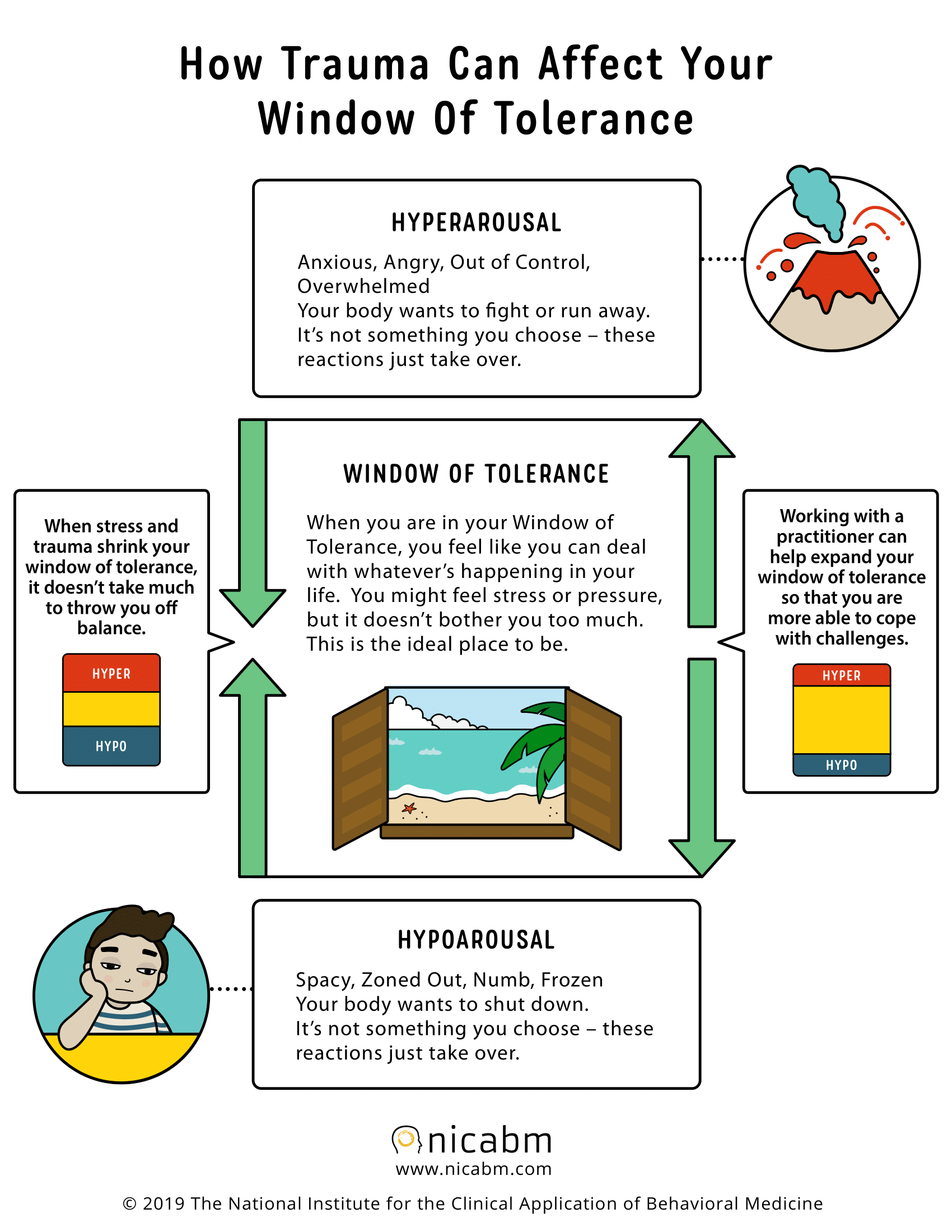
Children and young people who have suffered abuse and neglect can seem to be experts at “pressing the buttons” of grown-ups, pushing them out of their Window of Tolerance. They have had to, to survive. Regardless of what we believe we have overcome in our past, those emotions inevitably resurface due to the nature of the work. Not the least of which is confronting the basic assumptions we have internalised through the culture, values, and beliefs of our own upbringing. In the residential group living context, these basic assumptions will be challenged. If this challenge can be accepted, it can be a tremendous learning experience and enable significant personal growth and self-awareness for workers.
It becomes even more difficult when you believe you cannot talk about it to colleagues or supervisors because they “just won’t get it”, or you feel like they will judge you. Sometimes, you may even be unaware of why you are angry. After all, you are doing this job because you are committed to making a difference in young people’s lives – and you do make a difference!
I don’t think any of us grow up without a few scars which remain dormant in most professional roles. We all like to think our set of skills contains amazing strengths, particularly in relation to being confronted by young people with extreme behaviours that challenge.
At the Centre for Excellence in Therapeutic Care, we changed the wording from “young people with challenging behaviours” to “young people with behaviours that challenge” because we recognise that we are all challenged by different behaviours at different times. Our behaviours are usually a product of our own life journeys, and everyone has a different journey.
Most of us recognise our triggers which touch fleetingly or deeply on pain we thought we had dealt with. What is hard to raise in reflective practice and supervision is the incredible anger, and even hatred, we can feel towards a young person. Training doesn’t prepare you for feeling it. We are so committed to loving and caring through building safe and trusting relationships with our children and young people, that experiencing feelings of anger, dislike, hatred, and retribution sandwiched between feelings of shame is totally foreign to us – but it does happen.
An example from my practice
A 17-year-old young man living in a residential unit that I managed worked on a chicken farm. I had to make a few decisions he did not like, due to his unprovoked and dangerous threats and actions towards workers and the other young people. He threatened me many times, but I stayed calm (I think). He tried to grab a police officer’s gun at the police station to “fix” me. The situation deteriorated to the stage where he would often walk past my office or see me in the street and make cutting actions across his throat whilst glaring at me and holding his gaze, even when past. What I didn’t know at the time, was that he was employed to kill chickens. On reflection, the young man appeared to be employing maladaptive coping mechanisms, including emotional detachment and resorting to violence to cope with the slaughter of the animals on a daily basis.
I let my dislike and anger guide my response to glare back and strut, demonstrating “I’m not afraid of you”. I did nothing to repair or even understand the behaviours that challenged me, and I have regretted it for 25 years.
Responses to case example
What did I do?
- I did nothing and have regretted it ever since
What could I have done?
- Discussed in Care Team meeting
- Develop a plan using double-rostering or additional staff
- Asked for support from supervisor and colleagues
- Met with the young man after seeking advice to try and establish a better relationship
- Unpacked my response in referred personal counselling
What would you have done and felt in these circumstances?
Triggers
Often our reactions come from a place deep inside us. We are not always consciously aware of our triggers until working directly with young people in our shared, intense, everyday life-space. We already know there is a (usually unconscious) reason behind every behaviour, even when it seems to come from nowhere. However, behaviours can take us by surprise when they seem unpredictable, upsetting normally calm people and set off strong and confusing reactions such as anger and hatred.

It is important to remember that we are all different with different life experiences, so we can’t predict who will react to what. In the intense environment of residential care, people behave and respond surprisingly differently. We can misread what others are saying and their intentions, overreact to certain personalities, or to personal issues inside us.
Additionally, our young people are extremely experienced at searching for, finding, and feeding our triggers and pain. They have had to, to survive. We may feel shame at feeling anger and hatred toward young people who exploit our triggers but often won’t talk about it or try to cover it up. When working closely with that young person, that shame can become perpetual, increasing the feeling of anger and even blame towards the young person.
We often do not know what will trigger us or our young people before escalation, making it difficult to plan for and grow from. A supportive organisational culture needs to enable workers to seek help without fear of retribution or being stood down – an inappropriate response unless someone is physically injured. The residential care system is not set up to understand these issues and is governed by risk-aversive policies.
Overcoming our emotional reactions
We need to get help to explore and better understand these intense feelings and responses and what caused them to develop support plans for agencies, workers and young people.
There may be many different preferred outcomes to resolving feeling hate and/or anger at a young person, which may include:
- Support from colleagues & Care Teams
- Support from Therapeutic Specialist and Supervisor
- Working with the young person
- Taking a short break from work
- Referral for ongoing personal counselling
- Where possible and agreed to be a positive move, transfer to another house after careful planning to avoid further shame
References
National Institute of the Clinical Application to Behavioral Medicine. (2019). How to Help Your Clients Understand Their Window of Tolerance [Infographic]. https://www.nicabm.com/trauma-how-to-help-your-clients-understand-their-window-of-tolerance/
Ward, A. (2014). Leadership in Residential Care: A Relationship-Based Approach. Smokehouse Press, Norwich.